In February 2017, ACOG released a committee opinion report titled “Approaches to Limit Intervention During Labor and Birth” which lists routine interventions that they think are not necessary or beneficial and should no longer be practiced. In addition, ACOG has acknowledged the role that caregivers play in the birth experience. They state, “Satisfaction with one’s birth experience also is related to personal expectations, support from caregivers, quality of the patient-caregiver relationship, and the patient’s involvement in decision making.” ACOG (The American College of Obstetricians and Gynecologists) sets guidelines that doctors and nurses follow, and their report is enough to make a skeptic feel optimistic.
ACOG’s NEW RECOMMENDATIONS:
Allow Women to Move/Change Position – The report states “Frequent position changes during labor to enhance maternal comfort and promote optimal fetal positioning can be supported.” ACOG recommends that no one position be prescribed over another, but they warn that women who labor on their backs can suffer additional complications. ACOG sites a study which concluded that women who labored in upright positions shortened their labors more effectively than augmenting labor with artificially rupturing membranes and administering oxytocin and were more likely to deliver vaginally. They mention that frequent position changes help the baby to get in optimal position for delivery.
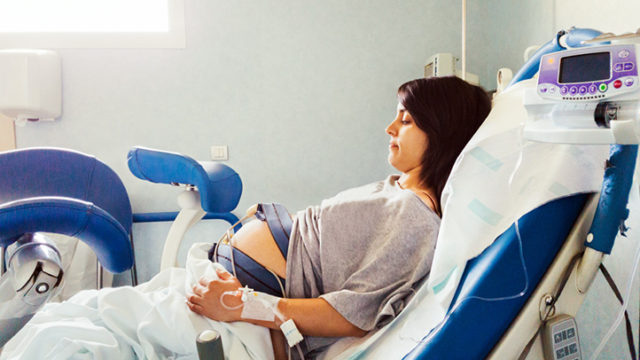
Use Intermittent Fetal Monitoring – They state intermittent heart-rate monitoring is as effective as continuous electronic fetal monitoring, and it allows freedom of movement for the laboring woman.
Support Natural Methods of Pain Relief and Coping – They state how pharmacologic methods can help relieve pain, but do not help with coping, or relieving anxiety or suffering. Some methods that they support for coping are water immersion, intradermal sterile water injections, relaxation techniques, acupuncture, massage, childbirth education, transcutaneous electrical nerve stimulation (TENS), aromatherapy, or audioanalgesia. They also state that having continuous support during labor helps women cope.
Let Women Push on Thier Own Accord – The report states “Obstetric care providers in the United States often encourage women in labor to push with a prolonged, closed glottis effort (ie, Valsalva maneuver) during each contraction. However, when not coached to breathe in a specific way, women push with an open glottis. Each woman should be encouraged to use the technique that she prefers and is most effective for her.”
Allow Hydration and Oral Intake During Labor – ACOG says, “Oral hydration can be encouraged to meet hydration and caloric needs.” Unfortunately, the committee remains uncertain about solid foods. ACOG says that routine IV fluids are not necessary when a woman is allowed oral intake.
Allow First-Time Mothers A 1-2Hour Rest Period After Dilation, Before Pushing – The report states “Offering nulliparous (first-time) women with epidural analgesia a rest period at 10 centimeters dilatation before pushing is based on the theory that a rest period allows the fetus to passively rotate and descend while conserving the woman’s energy for pushing efforts. This practice is called delayed pushing, laboring down, or passive descent.”
Women Do Not Need Admitted to the Hospital Before Active Labor – ACOG states “When women are observed or admitted for pain or fatigue in latent labor, techniques such as education and support, oral hydration, positions of comfort, and nonpharmacologic pain management techniques such as massage or water immersion may be beneficial.” They state it could take up to 28 hours for a woman to go into labor after her water has broken, so her care provider should help her manage her labor instead of admitting and inducing her. However, they state care providers will need to administer antibiotics and may choose to induce a woman who is Strep B positive.
Continuous Support During Labor: Family, Doulas, Nurses – In their own words, “Evidence suggests that, in addition to regular nursing care, the continuous one-to-one emotional support provided by support personnel, such as a doula, is associated with improved outcomes for women in labor. Benefits found in randomized trials include shortened labor, decreased need for analgesia, fewer operative deliveries, and fewer reports of dissatisfaction with the experience of labor.”
Routine Amniotomy (Artificial Rupture of Membranes/Waters) — ACOG states how the practice of artificially breaking a woman’s water is questionable.
In conclusion, ACOG acknowledges how current medical practices are harmful to a woman’s birth experience and psyche. Women have felt disrespected and even assaulted during childbirth and many fear the treatment they may receive from their hospital more than any other aspect of childbirth. We will have to see how these suggestions will be reflected in the hospital setting, but hopefully, the days where doctors and nurses look at natural birth plans in scorn will be over soon.